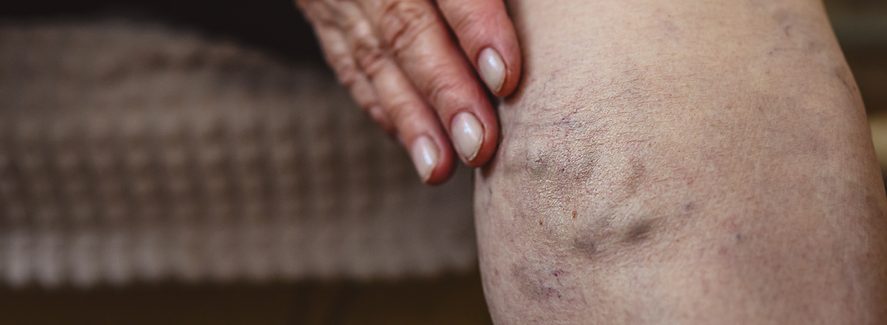
Do I Have Vein Disease? Vein disease may cause aggravating symptoms including: Itching Heaviness/tiredness Aches/pain/tenderness Burning Numbness/Tingling Night cramping Restless legs Vein disease may cause visible signs including: Spider veins -- especially below your knees or near your ankles Bulging, varicose veins Ankle swelling Skin discoloration…
CMO Vein911February 29, 2024